|
|
Ibanez-Rosello, B., Bautista-Ballesteros, J. A., Candela-Juan, C., Villaescusa, J. I., Ballester, F., Vijande, J., et al. (2017). Evaluation of the shielding in a treatment room with an electronic brachytherapy unit. J. Radiol. Prot., 37(2), N5–N12.
Abstract: Esteya (R) (Elekta Brachytherapy, Veenendaal, The Netherlands) is an electronic brachytherapy (eBT) system based on a 69.5 kVp x-ray source and a set of collimators of 1 to 3 cm in diameter, used for treating non-melanoma skin cancer lesions. This study aims to estimate room shielding requirements for this unit. The non-primary (scattered and leakage) ambient dose equivalent rates were measured with a Berthold LB-133 monitor (Berthold Technologies, Bad Wildbad, Germany). The latter ranges from 17 mSv h(-1) at 0.25 m distance from the x-ray source to 0.1 mSv h(-1) at 2.5 m. The necessary room shielding was then estimated following US and some European guidelines. The room shielding for all barriers considered was below 2 mmPb. The dose to a companion who, exceptionally, would stay with the patient during all treatment was estimated to be below 1 mSv if a leaded apron is used. In conclusion, Esteya shielding requirements are minimal.
|
|
|
|
Granero, D., Vijande, J., Ballester, F., & Rivard, M. J. (2011). Dosimetry revisited for the HDR Ir-192 brachytherapy source model mHDR-v2. Med. Phys., 38(1), 487–494.

Abstract: Purpose: Recently, the manufacturer of the HDR Ir-192 mHDR-v2 brachytherapy source reported small design changes (referred to herein as mHDR-v2r) that are within the manufacturing tolerances but may alter the existing dosimetric data for this source. This study aimed to (1) check whether these changes affect the existing dosimetric data published for this source; (2) obtain new dosimetric data in close proximity to the source, including the contributions from 192Ir electrons and considering the absence of electronic equilibrium; and (3) obtain scatter dose components for collapsed cone treatment planning system implementation. Methods: Three different Monte Carlo (MC) radiation transport codes were used: MCNP5, PENELOPE2008, and GEANT4. The source was centrally positioned in a 40 cm radius water phantom. Absorbed dose and collision kerma were obtained using 0.1 mm (0.5 mm) thick voxels to provide high-resolution dosimetry near (far from) the source. Dose-rate distributions obtained with the three MC codes were compared. Results: Simulations of mHDR-v2 and mHDR-v2r designs performed with three radiation transport codes showed agreement typically within 0.2% for r >= 0.25 cm. Dosimetric contributions from source electrons were significant for r<0.25 cm. The dose-rate constant and radial dose function were similar to those from previous MC studies of the mHDR-v2 design. The 2D anisotropy function also coincided with that of the mHDR-v2 design for r >= 0.25 cm. Detailed results of dose distributions and scatter components are presented for the modified source design. Conclusions: Comparison of these results to prior MC studies showed agreement typically within 0.5% for r >= 0.25 cm. If dosimetric data for r<0.25 cm are not needed, dosimetric results from the prior MC studies will be adequate. c 2011 American Association of Physicists in Medicine.
|
|
|
|
Quintero-Quintero, A., Patiño-Camargo, G., Soriano, A., Palma, J. D., Vilar-Palop, J., Pujades, M. C., et al. (2018). Calibration of a thermoluminescent dosimeter worn over lead aprons in fluoroscopy guided procedures. J. Radiol. Prot., 38(2), 549–563.

Abstract: Fluoroscopy guided interventional procedures provide remarkable benefits to patients. However, medical staff working near the scattered radiation field may be exposed to high cumulative equivalent doses, thus requiring shielding devices such as lead aprons and thyroid collars. In this situation, it remains an acceptable practice to derive equivalent doses to the eye lenses or other unprotected soft tissues with a dosimeter placed above these protective devices. Nevertheless, the radiation backscattered by the lead shield differs from that generated during dosimeter calibration with a water phantom. In this study, a passive personal thermoluminescent dosimeter (TLD) was modelled by means of the Monte Carlo (MC) code Penelope. The results obtained were validated against measurements performed in reference conditions in a secondary standard dosimetry laboratory. Next, the MC model was used to evaluate the backscatter correction factor needed for the case where the dosimeter is worn over a lead shield to estimate the personal equivalent dose H-p(0.07) to unprotected soft tissues. For this purpose, the TLD was irradiated over a water slab phantom with a photon beam representative of the result of a fluoroscopy beam scattered by a patient. Incident beam angles of 0 degrees and 60 degrees, and lead thicknesses between the TLD and phantom of 0.25 and 0.5 mm Pb were considered. A backscatter correction factor of 1.23 (independent of lead thickness) was calculated comparing the results with those faced in reference conditions (i.e., without lead shield and with an angular incidence of 0 degrees). The corrected dose algorithm was validated in laboratory conditions with dosi-meters irradiated over a thyroid collar and angular incidences of 0 degrees, 40 degrees and 60 degrees, as well as with dosimeters worn by interventional radiologists and cardiologists. The corrected dose algorithm provides a better approach to estimate the equivalent dose to unprotected soft tissues such as eye lenses. Dosimeters that are not shielded from backscatter radiation might underestimate personal equivalent doses when worn over a lead apron and, therefore, should be specifically characterized for this purpose.
|
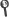
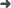
|
|
|
Garcia-Cases, F., Perez-Calatayud, J., Ballester, F., Vijande, J., & Granero, D. (2018). Peripheral dose around a mobile linac for intraoperative radiotherapy: radiation protection aspects. J. Radiol. Prot., 38(4), 1393–1411.

Abstract: The aim of this work is to analyse the scattered radiation produced by the mobile accelerator Mobetron 1000. To do so, detailed Monte Carlo simulations using two different codes, Penelope2008 and Geant4, were performed. Measurements were also done. To quantify the attenuation due to the internal structures, present in the accelerator head, on the scattered radiation produced, some of the main structural shielding in the Mobetron 1000 has been incorporated into the geometry simulation. Results are compared with measurements. Some discrepancies between the calculated and measured dose values were found. These differences can be traced back to the importance of the radiation component due to low energy scattered electrons. This encouraged us to perform additional calculations to separate the role played by this component. Ambient dose equivalent, H*(10), outside of the operating room (OR) has been evaluated using Geant4. H*(10) has been measured inside and outside the OR, being its values compatible with those reported in the literature once the low energy electron component is removed. With respect to the role played by neutrons, estimations of neutron H*(10) using Geant4 together with H*(10) measurements has been performed for the case of the 12 MeV electron beam. The values obtained agree with the experimental values existing in the literature, being much smaller than those registered in conventional accelerators. This study is a useful tool for the clinical user to investigate the radiation protection issues arising with the use of these accelerators in ORs without structural shielding. These results will also enable to better fix the maximum number of treatments that could be performed while insuring adequate radiological protection of workers and public in the hospital.
|
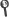
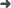
|
|
|
Granero, D., Perez-Calatayud, J., Vijande, J., Ballester, F., & Rivard, M. J. (2014). Limitations of the TG-43 formalism for skin high-dose-rate brachytherapy dose calculations. Med. Phys., 41(2), 021703–8pp.

Abstract: Purpose: In skin high-dose-rate (HDR) brachytherapy, sources are located outside, in contact with, or implanted at some depth below the skin surface. Most treatment planning systems use the TG-43 formalism, which is based on single-source dose superposition within an infinite water medium without accounting for the true geometry in which conditions for scattered radiation are altered by the presence of air. The purpose of this study is to evaluate the dosimetric limitations of the TG-43 formalism in HDR skin brachytherapy and the potential clinical impact. Methods: Dose rate distributions of typical configurations used in skin brachytherapy were obtained: a 5 cm x 5 cm superficial mould; a source inside a catheter located at the skin surface with and without backscatter bolus; and a typical interstitial implant consisting of an HDR source in a catheter located at a depth of 0.5 cm. Commercially available HDR Co-60 and Ir-192 sources and a hypothetical Yb-169 source were considered. The Geant4Monte Carlo radiation transport code was used to estimate dose rate distributions for the configurations considered. These results were then compared to those obtained with the TG-43 dose calculation formalism. In particular, the influence of adding bolus material over the implant was studied. Results: For a 5 cm x 5 cm Ir-192 superficial mould and 0.5 cm prescription depth, dose differences in comparison to the TG-43 method were about -3%. When the source was positioned at the skin surface, dose differences were smaller than -1% for Co-60 and Ir-192, yet -3% for Yb-169. For the interstitial implant, dose differences at the skin surface were -7% for Co-60, -0.6% for Ir-192, and -2.5% for Yb-169. Conclusions: This study indicates the following: (i) for the superficial mould, no bolus is needed; (ii) when the source is in contact with the skin surface, no bolus is needed for either Co-60 and Ir-192. For lower energy radionuclides like Yb-169, bolus may be needed; and (iii) for the interstitial case, at least a 0.1 cm bolus is advised for Co-60 to avoid underdosing superficial target layers. For Ir-192 and Yb-169, no bolus is needed. For those cases where no bolus is needed, its use might be detrimental as the lack of radiation scatter may be beneficial to the patient, although the 2% tolerance for dose calculation accuracy recommended in the AAPM TG-56 report is not fulfilled.
|
|

