|
|
Calatayud-Jordan, J., Candela-Juan, C., Palma, J. D., Pujades-Claumarchirant, M. C., Soriano, A., Gracia-Ochoa, M., et al. (2021). Influence of the simultaneous calibration of multiple ring dosimeters on the individual absorbed dose. J. Radiol. Prot., 41(2), 384–397.

Abstract: Ring dosimeters for personal dosimetry are calibrated in accredited laboratories following ISO 4037-3 guidelines. The simultaneous irradiation of multiple dosimeters would save time, but has to be carefully studied, since the scattering conditions could change and influence the absorbed dose in nearby dosimeters. Monte Carlo simulations using PENELOPE-2014 were performed to explore the need to increase the uncertainty of H-p (0.07) in the simultaneous irradiation of three and five DXT-RAD 707H-2 (Thermo Scientific) ring dosimeters with beam qualities: N-30, N-80 and N-300. Results show that the absorbed dose in each dosimeter is compatible with each of the others and with the reference simulation (a single dosimeter), with a coverage probability of 95% (k = 2). Comparison with experimental data yielded consistent results with the same coverage probability. Therefore, five ring dosimeters can be simultaneously irradiated with beam qualities ranging, at least, between N-30 and N-300 with a negligible impact on the uncertainty of H-p (0.07).
|
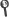
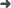
|
|
|
Assam, I., Vijande, J., Ballester, F., Perez-Calatayud, J., Poppe, B., & Siebert, F. A. (2022). Evaluation of dosimetric effects of metallic artifact reduction and tissue assignment on Monte Carlo dose calculations for I-125 prostate implants. Med. Phys., 49, 6195–6208.

Abstract: Purpose Monte Carlo (MC) simulation studies, aimed at evaluating the magnitude of tissue heterogeneity in I-125 prostate permanent seed implant brachytherapy (BT), customarily use clinical post-implant CT images to generate a virtual representation of a realistic patient model (virtual patient model). Metallic artifact reduction (MAR) techniques and tissue assignment schemes (TAS) are implemented on the post-implant CT images to mollify metallic artifacts due to BT seeds and to assign tissue types to the voxels corresponding to the bright seed spots and streaking artifacts, respectively. The objective of this study is to assess the combined influence of MAR and TAS on MC absorbed dose calculations in post-implant CT-based phantoms. The virtual patient models used for I-125 prostate implant MC absorbed dose calculations in this study are derived from the CT images of an external radiotherapy prostate patient without BT seeds and prostatic calcifications, thus averting the need to implement MAR and TAS. Methods The geometry of the IsoSeed I25.S17plus source is validated by comparing the MC calculated results of the TG-43 parameters for the line source approximation with the TG-43U1S2 consensus data. Four MC absorbed dose calculations are performed in two virtual patient models using the egs_brachy MC code: (1) TG-43-based D-w,w-TG(43), (2) D-w,D-w-MBDC that accounts for interseed scattering and attenuation (ISA), (3) D-m,D-m that examines ISA and tissue heterogeneity by scoring absorbed dose in tissue, and (4) D-w,D-m that unlike D-m,D-m scores absorbed dose in water. The MC absorbed doses (1) and (2) are simulated in a TG-43 patient phantom derived by assigning the densities of every voxel to 1.00 g cm(-3) (water), whereas MC absorbed doses (3) and (4) are scored in the TG-186 patient phantom generated by mapping the mass density of each voxel to tissue according to a CT calibration curve. The MC absorbed doses calculated in this study are compared with VariSeed v8.0 calculated absorbed doses. To evaluate the dosimetric effect of MAR and TAS, the MC absorbed doses of this work (independent of MAR and TAS) are compared to the MC absorbed doses of different I-125 source models from previous studies that were calculated with different MC codes using post-implant CT-based phantoms generated by implementing MAR and TAS on post-implant CT images. Results The very good agreement of TG-43 parameters of this study and the published consensus data within 3% validates the geometry of the IsoSeed I25.S17plus source. For the clinical studies, the TG-43-based calculations show a D-90 overestimation of more than 4% compared to the more realistic MC methods due to ISA and tissue composition. The results of this work generally show few discrepancies with the post-implant CT-based dosimetry studies with respect to the D-90 absorbed dose metric parameter. These discrepancies are mainly Type B uncertainties due to the different I-125 source models and MC codes. Conclusions The implementation of MAR and TAS on post-implant CT images have no dosimetric effect on the I-125 prostate MC absorbed dose calculation in post-implant CT-based phantoms.
|
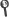
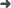
|
|
|
Perez-Calatayud, J., Ballester, F., Tedgren, C., DeWerd, L. A., Papagiannis, P., Rivard, M. J., et al. (2022). GEC-ESTRO ACROP recommendations on calibration and traceability of HE HDR-PDR photon-emitting brachytherapy sources at the hospital level. Radiother. Oncol., 176, 108–117.
Abstract: The vast majority of radiotherapy departments in Europe using brachytherapy (BT) perform temporary implants of high-or pulsed-dose rate (HDR-PDR) sources with photon energies higher than 50 keV. Such techniques are successfully applied to diverse pathologies and clinical scenarios. These recommen-dations are the result of Working Package 21 (WP-21) initiated within the BRAchytherapy PHYsics Quality Assurance System (BRAPHYQS) GEC-ESTRO working group with a focus on HDR-PDR source cal-ibration. They provide guidance on the calibration of such sources, including practical aspects and issues not specifically accounted for in well-accepted societal recommendations, complementing the BRAPHYQS WP-18 Report dedicated to low energy BT photon emitting sources (seeds). The aim of this report is to provide a European-wide standard in HDR-PDR BT source calibration at the hospital level to maintain high quality patient treatments.
|
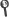
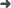
|
|
|
Oliver, S., Vijande, J., Tejedor-Aguilar, N., Miro, R., Rovira-Escutia, J. J., Ballester, F., et al. (2023). Monte Carlo flattening filter design to high energy intraoperative electron beam homogenization. Radiat. Phys. Chem., 212, 111102–6pp.

Abstract: Intraoperative radiotherapy using mobile linear accelerators is used for a wide variety of malignancies. However, when large fields are used in combination with high energies, a deterioration of the flatness dose profile is measured with respect to smaller fields and lower energies. Indeed, for the LIAC HWL of Sordina, this deterioration is observed for the 12 MeV beam combined with 10 cm (or larger) diameter applicator. Aimed to solve this problem, a flattening filter has been designed and validated evaluating the feasibility of its usage at the upper part of the applicator. The design of the filter was based on Monte Carlo simulations because of its accuracy in modeling components of clinical devices, among other purposes. The LIAC 10 cm diameter applicator was modeled and simulated independently by two different research groups using two different MC codes, reproducing the heterogeneity of the 12 MeV energy beam. Then, an iterative process of filter design was carried out. Finally, the MC designed conical filter with the optimal size and height to obtain the desired flattened beam was built in-house using a 3D printer. During the experimental validation of the applicator-filter, percentage depth dose, beam profiles, absolute and peripheral dose measurements were performed to demonstrate the effectiveness of the filter addition in the applicator. These measurements conclude that the beam has been flattened, from 5.9% with the standard configuration to 1.6% for the configuration with the filter, without significant increase of the peripheral dose. Consequently, the new filter-applicator LIAC configuration can be used also in a conventional surgery room. A reduction of 16% of the output dose and a reduction of 1.1 mm in the D50 of the percentage depth dose was measured with respect to the original configuration. This work is a proof-of-concept that demonstrates that it is possible to add a filter able to flatten the beam delivered by the Sordina LIAC HWL. Future studies will focus on more refined technical solutions fully compatible with the integrity of the applicator, including its sterilization, to be safely introduced in the clinical practice.
|
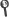
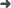
|
|
|
Piriz, G. H., Gonzalez-Sprinberg, G. A., Ballester, F., & Vijande, J. (2024). Dosimetry of Large Field Valencia applicators for Cobalt-60-based brachytherapy. Med. Phys., 51, 5094–5098.

Abstract: BackgroundNon-melanoma skin cancer is one of the most common types of cancer and one of the main approaches is brachytherapy. For small lesions, the treatment of this cancer with brachytherapy can be done with two commercial applicators, one of these is the Large Field Valencia Applicators (LFVA).PurposeThe aim of this study is to test the capabilities of the LFVA to use clinically 60Co sources instead of the 192Ir ones. This study was designed for the same dwell positions and weights for both sources.MethodsThe Penelope Monte Carlo code was used to evaluate dose distribution in a water phantom when a 60Co source is considered. The LFVA design and the optimized dwell weights reported for the case of 192Ir are maintained with the only exception of the dwell weight of the central position, that was increased. 2D dose distributions, field flatness, symmetry and the leakage dose distribution around the applicator were calculated.ResultsWhen comparing the dose distributions of both sources, field flatness and symmetry remain unchanged. The only evident difference is an increase of the penumbra regions for all depths when using the 60Co source. Regarding leakage, the maximum dose within the air volume surrounding the applicator is in the order of 20% of the prescription dose for the 60Co source, but it decreases to less than 5% at about 1 cm distance.ConclusionsFlatness and symmetry remains unaltered as compared with 192Ir sources, while an increase in leakage has been observed. This proves the feasibility of using the LFVA in a larger range of clinical applications.
|
|

