|
|
Palomo, R., Pujades, M. C., Gimeno-Olmos, J., Carmona, V., Lliso, F., Candela-Juan, C., et al. (2015). Evaluation of lens absorbed dose with Cone Beam IGRT procedures. J. Radiol. Prot., 35(4), N33–N41.

Abstract: The purpose of this work is to evaluate the absorbed dose to the eye lenses due to the cone beam computed tomography (CBCT) system used to accurately position the patient during head-and-neck image guided procedures. The on-board imaging (OBI) systems (v. 1.5) of Clinac iX and TrueBeam (Varian) accelerators were used to evaluate the imparted dose to the eye lenses and some additional points of the head. All CBCT scans were acquired with the Standard-Dose Head protocol from Varian. Doses were measured using thermoluminescence dosimeters (TLDs) placed in an anthropomorphic phantom. TLDs were calibrated at the beam quality used to reduce their energy dependence. Average dose to the lens due to the OBI systems of the Clinac iX and the TrueBeam were 0.71 +/- 0.07 mGy/CBCT and 0.70 +/- 0.08 mGy/CBCT, respectively. The extra absorbed dose received by the eye lenses due to one CBCT acquisition with the studied protocol is far below the 500 mGy threshold established by ICRP for cataract formation (ICRP 2011 Statement on Tissue Reactions). However, the incremental effect of several CBCT acquisitions during the whole treatment should be taken into account.
|
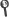
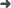
|
|
|
Pujades, M. C., Granero, D., Vijande, J., Ballester, F., Perez-Calatayud, J., Papagiannis, P., et al. (2014). Air-kerma evaluation at the maze entrance of HDR brachytherapy facilities. J. Radiol. Prot., 34(4), 741–753.

Abstract: In the absence of procedures for evaluating the design of brachytherapy (BT) facilities for radiation protection purposes, the methodology used for external beam radiotherapy facilities is often adapted. The purpose of this study is to adapt the NCRP 151 methodology for estimating the air-kerma rate at the door in BT facilities. Such methodology was checked against Monte Carlo (MC) techniques using the code Geant4. Five different facility designs were studied for Ir-192 and Co-60 HDR applications to account for several different bunker layouts. For the estimation of the lead thickness needed at the door, the use of transmission data for the real spectra at the door instead of the ones emitted by Ir-192 and Co-60 will reduce the lead thickness by a factor of five for Ir-192 and ten for Co-60. This will significantly lighten the door and hence simplify construction and operating requirements for all bunkers. The adaptation proposed in this study to estimate the air-kerma rate at the door depends on the complexity of the maze: it provides good results for bunkers with a maze (i.e. similar to those used for linacs for which the NCRP 151 methodology was developed) but fails for less conventional designs. For those facilities, a specific Monte Carlo study is in order for reasons of safety and cost-effectiveness.
|
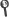
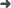
|
|
|
Quintero-Quintero, A., Patiño-Camargo, G., Soriano, A., Palma, J. D., Vilar-Palop, J., Pujades, M. C., et al. (2018). Calibration of a thermoluminescent dosimeter worn over lead aprons in fluoroscopy guided procedures. J. Radiol. Prot., 38(2), 549–563.

Abstract: Fluoroscopy guided interventional procedures provide remarkable benefits to patients. However, medical staff working near the scattered radiation field may be exposed to high cumulative equivalent doses, thus requiring shielding devices such as lead aprons and thyroid collars. In this situation, it remains an acceptable practice to derive equivalent doses to the eye lenses or other unprotected soft tissues with a dosimeter placed above these protective devices. Nevertheless, the radiation backscattered by the lead shield differs from that generated during dosimeter calibration with a water phantom. In this study, a passive personal thermoluminescent dosimeter (TLD) was modelled by means of the Monte Carlo (MC) code Penelope. The results obtained were validated against measurements performed in reference conditions in a secondary standard dosimetry laboratory. Next, the MC model was used to evaluate the backscatter correction factor needed for the case where the dosimeter is worn over a lead shield to estimate the personal equivalent dose H-p(0.07) to unprotected soft tissues. For this purpose, the TLD was irradiated over a water slab phantom with a photon beam representative of the result of a fluoroscopy beam scattered by a patient. Incident beam angles of 0 degrees and 60 degrees, and lead thicknesses between the TLD and phantom of 0.25 and 0.5 mm Pb were considered. A backscatter correction factor of 1.23 (independent of lead thickness) was calculated comparing the results with those faced in reference conditions (i.e., without lead shield and with an angular incidence of 0 degrees). The corrected dose algorithm was validated in laboratory conditions with dosi-meters irradiated over a thyroid collar and angular incidences of 0 degrees, 40 degrees and 60 degrees, as well as with dosimeters worn by interventional radiologists and cardiologists. The corrected dose algorithm provides a better approach to estimate the equivalent dose to unprotected soft tissues such as eye lenses. Dosimeters that are not shielded from backscatter radiation might underestimate personal equivalent doses when worn over a lead apron and, therefore, should be specifically characterized for this purpose.
|
|

